Auto logout in seconds.
Continue LogoutExecutive summary
Healthcare organizations are operating in an increasingly complex environment. Changes in how care is delivered and what leaders prioritize are reshaping operations and the systems that support them. At the same time, persistent cost pressures, workforce and demographic shifts, and evolving policy requirements continue to complicate planning and execution across the healthcare ecosystem.
For executive leaders responsible for procurement and supply chain performance, this moment represents a strategic inflection point. Ensuring reliable access to products while managing ongoing cost pressures now requires more deliberate, system‑wide approaches. As health systems expand and invest in innovation, procurement teams are being asked to deliver greater efficiency and standardization, supported by targeted technology investments that enable consistency and scale, all without disrupting care delivery or business operations.
This report analyzes results from our national survey of 102 health system supply chain and executive leaders and examines:
- The current state of healthcare procurement
- Challenges shaping procurement functions
- Approaches supply chain teams are using to adapt
- Efforts to foster a no-disruption environment
Top 5 procurement challenges and objectives
Rising costs emerged as the most frequently cited challenge procurement leaders say they expect to face in 2026. This finding is not surprising given uncertainty surrounding tariffs, ongoing margin pressures, and federal policy changes that could lead to cuts to Medicaid and other funding.
What is notable, however, is how leaders say they are responding to these pressures. Rather than defaulting to blunt cost‑cutting measures, most are pursuing balanced strategies that protect both financial performance and operational effectiveness. Leaders are focused on approaches that align cost control with broader supply chain objectives.
These strategies include:
- Ensuring clinicians and patients have access to high‑quality, reliable products
- Standardizing vendors and SKUs to increase scale and simplify operations
- Strengthening supply chain resilience to better withstand future disruptions
- Improving inventory visibility and management to reduce waste and variability
Success will depend on a mix of disciplined execution, selective adoption of new tools or technologies, and deeper collaboration with suppliers and other supply chain partners.
| Top challenges for health system supply chain leaders1 | |
|---|---|
1. Rising costs | 60% |
2. Predictability of product demand | 42% |
3. Managing multiple vendors | 36% |
4. Complexity of inventory management | 31% |
5. Regulatory compliance and reporting | 24% |
1 Percentages represent the proportion of respondents who included each item among their top three challenges or objectives. | |
| Most critical objectives for health system supply chain leaders1 | |
|---|---|
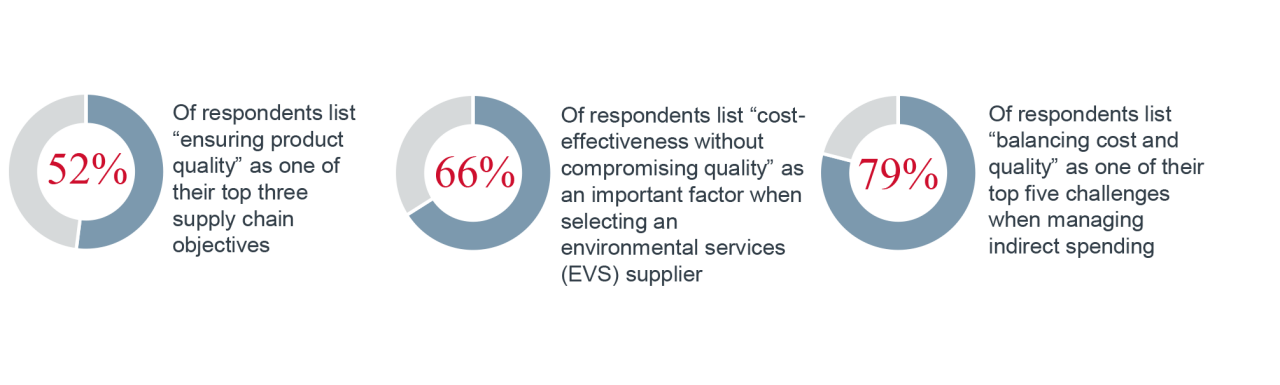
1. Ensuring product quality | 52% |
2. Optimizing inventory levels | 39% |
3. Consolidating supplier relationships | 34% |
4. Enhancing supply chain resilience | 32% |
5. Reducing overall costs | 31% |
1 Percentages represent the proportion of respondents who included each item among their top three challenges or objectives. | |
5 insights on healthcare procurement in 2026
The challenges and objectives on the previous page serve as the backdrop for five key insights that point to where procurement leaders are focusing in 2026 and beyond as they navigate a more turbulent healthcare environment.
What’s the context?
Standardization has long been a core procurement priority for health systems. As organizations have grown in size and faced sustained margin pressure, consolidating vendors and SKUs has delivered meaningful financial impact, with many health systems realizing millions of dollars in savings. These efforts have also helped reduce care variation, strengthen purchasing leverage, and simplify supply chain operations.
Of respondents list “controlling rogue spending” as one of their top five challenge in managing indirect spending
While many organizations have already captured the most accessible savings, additional opportunities remain. Even highly disciplined organizations continue to encounter structural and operational gaps that limit the full potential of standardization efforts.
Common reasons health systems continue to find standardization opportunities
"Health systems are focused not only on standardizing vendors and SKUs, but increasingly on standardizing the purchasing process itself. As organizations adopt platforms such as Workday, Ariba, Oracle, and GHX to consolidate spend and improve visibility, integration becomes critical. Staples integrates seamlessly with these procurement systems, helping drive efficiency, control vendor complexity, and create greater transparency across categories."
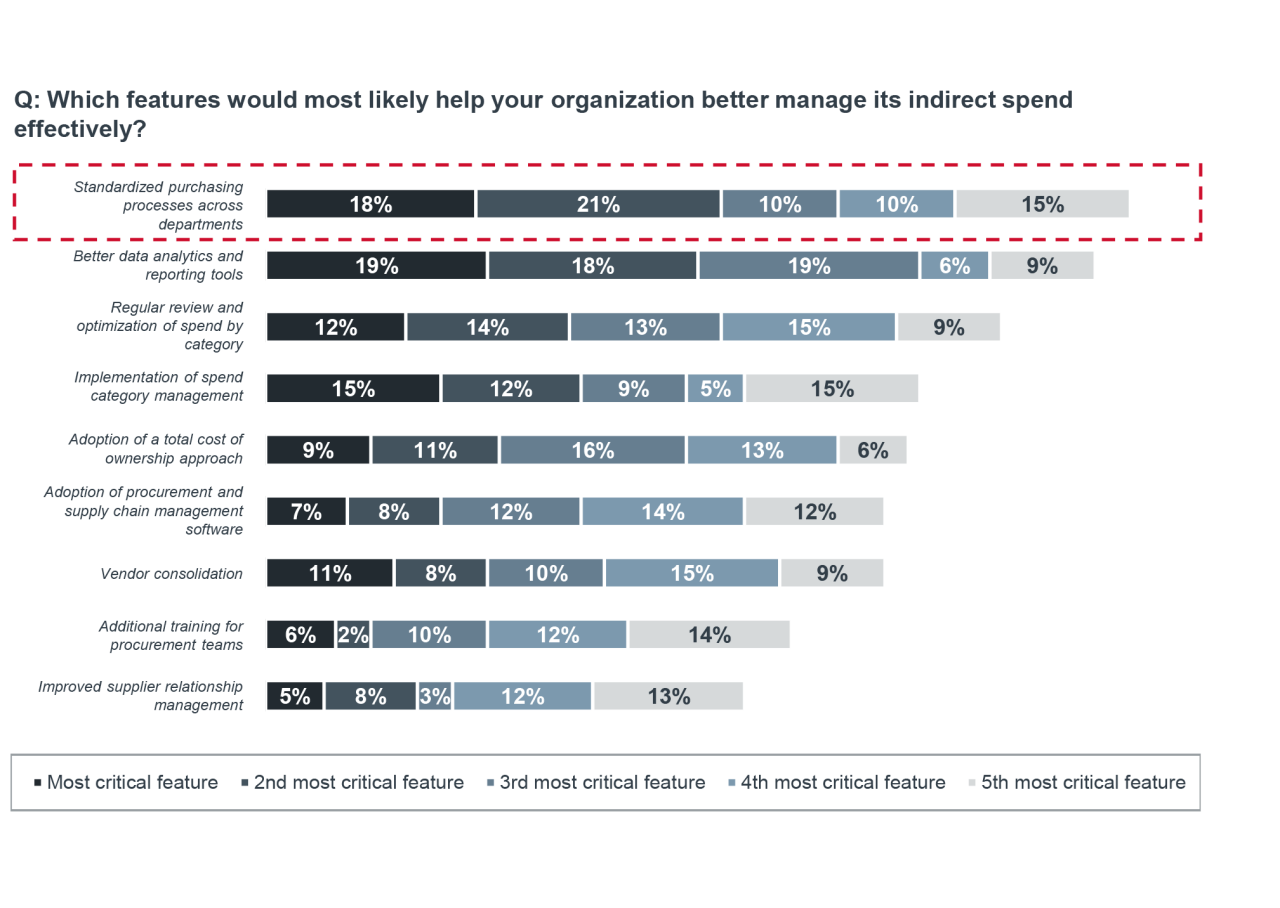
What’s happening in purchasing today?
Facing renewed margin pressure alongside continued organizational growth, health systems are revisiting standardization efforts as a lever for additional savings. This next phase of standardization is less about broad consolidation and more about targeted refinement, such as identifying sites or practices that exceed spend benchmarks, standardizing purchasing across additional product categories, or working with vendors that offer a broad portfolio of products across categories.
Health systems are also looking to expand standardization efforts beyond simply reducing the number of vendors or SKUs. Many are finding additional savings by aligning purchasing processes to support long‑term, repeatable success. These process‑focused approaches are designed to embed standardization into day‑to‑day operations, rather than treating it as a one‑time initiative.
Key opportunities to drive this next phase of standardization:
- Centralizing the procurement function at the system level
- Aligning purchasing workflows across ambulatory sites with the broader health system
- Matching data infrastructure across sites, including EHRs and enterprise research planning (ERP)
- Automating purchase order workflows to reduce manual effort and variability
- Standardizing request for proposal (RFP) templates to streamline sourcing and improve comparability
What’s the context?
The COVID‑19 pandemic and other logistical disruptions in the early 2020s exposed substantial vulnerabilities across the healthcare supply chain. Shortages, delays, and stockouts underscored how fragile sourcing and distribution models had become. In response, health systems across the country moved quickly to make supply chain resilience a strategic priority rather than a secondary operational concern.
To strengthen resilience, organizations expanded the number of vendors they rely on for critical items, reducing dependence on any single source. Others invested in deeper, more collaborative partnerships with suppliers to improve visibility and ensure continuity of supply during periods of disruption. In some cases, health systems went a step further by dedicating full‑time roles to supply chain resilience, signaling that preparedness and risk mitigation should not sit on the margins of leadership responsibilities. These efforts are intended to help organizations better withstand future disruptions, whether caused by natural disasters, labor actions, or other public health emergencies.
"We recognize that for the foreseeable future, supply chains will need to operate in a complex world with overlapping disruptions. In response, we have made inventory investments and advanced our technology to increase agility. These strategic investments are not just about adapting; they are fundamentally focused on safeguarding the customer experience. We now can deliver a 99%+ fulfillment experience even if there are disruptions."
What’s happening in purchasing today?
The most common way health systems are strengthening supply chain resilience today is by optimizing internal processes. Many organizations are focusing first on improvements they can control directly, using better data and more disciplined operating practices to reduce risk and variability across their supply chains. Common internal actions include:
- Developing more accurate demand forecasts
- Investing in analytics that provide greater visibility into inventory levels
- Adjusting storage and delivery strategies based on whether items are classified as critical or noncritical
These investments are designed to improve resilience while also driving efficiency. By strengthening internal capabilities, health systems can reduce the need to choose between business continuity and cost savings — they can support both objectives simultaneously.
When it comes to upstream supply chain resilience, health systems continue to rely on their GPO, distributor, and manufacturer partners. In these relationships, organizations are prioritizing partners who can offer diverse manufacturing or warehousing footprints, as well as stronger capabilities to anticipate and react to disruptions.
While it is possible for health systems to develop this level of upstream visibility on their own, many struggle with the cost and data limitations required to do so. As a result, supplier partnerships remain a primary path for gaining broader insight and resilience across the supply chain.
Of respondents list “optimizing inventory levels” as one of their top supply chain objectives
Of respondents list “reliability of the supply chain” among the most important factors when selecting an EVS supplier
Of respondents list “preparing for supply chain disruptions” as one of their top supply chain objectives
"When suppliers demonstrate strong resiliency planning, we have greater confidence in their long-term reliability and partnership."
What’s the context?
Health system sustainability efforts accelerated in the early 2020s, driven by a combination of financial incentives and public expectations. Many organizations pursued environmentally friendly initiatives in purchasing, benefiting from subsidies while also strengthening their reputations by highlighting their commitment to sustainability.
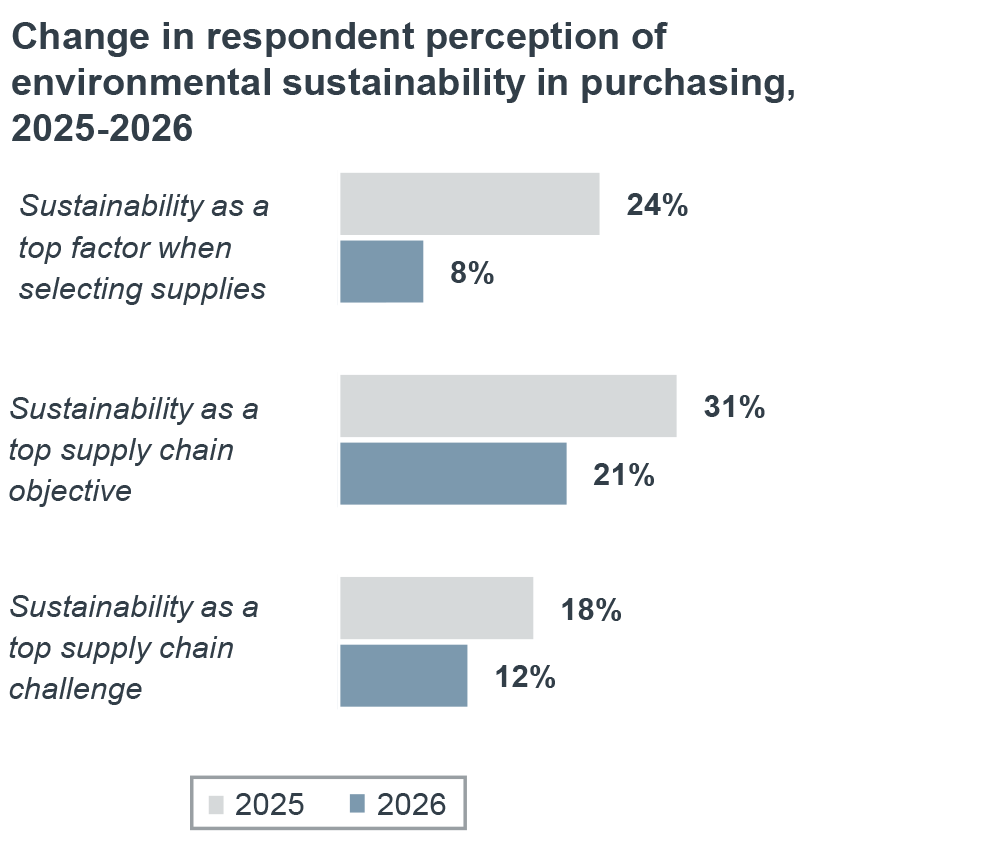
What’s happening in purchasing today?
Recently, many health systems have scaled back environmental sustainability initiatives. With leadership attention focused on margin preservation and care performance, sustainability efforts have become harder to prioritize. This shift has been reinforced by changes in the federal administration, which have reduced government incentives and funding for climate‑focused initiatives, further limiting the resources available to support these programs.
Although emerging pressures have taken priority over the past year, leaders continue to see environmental sustainability as pillar of broader supply chain success. Many health systems recognize that sustainability initiatives can support both environmental and financial performance at the same time, particularly when they are closely tied to efficiency and waste reduction.
In practice, organizations are finding opportunities to advance both objectives by:
- Eliminating supply waste that drives unnecessary spend and may ultimately end up in landfills
- Remanufacturing or repurposing products to reduce costs while extending the useful life of equipment
"At Stanford, sustainability is woven into our Supply Chain strategy via a focused SC-specific sustainability roadmap. By prioritizing responsible use, supplier partnerships, waste diversion, and chemicals of concern governance, we achieve fewer discarded products, lower costs, reduced variability, and a reduced landfill footprint — without compromising patient safety or care quality."
What’s the context?
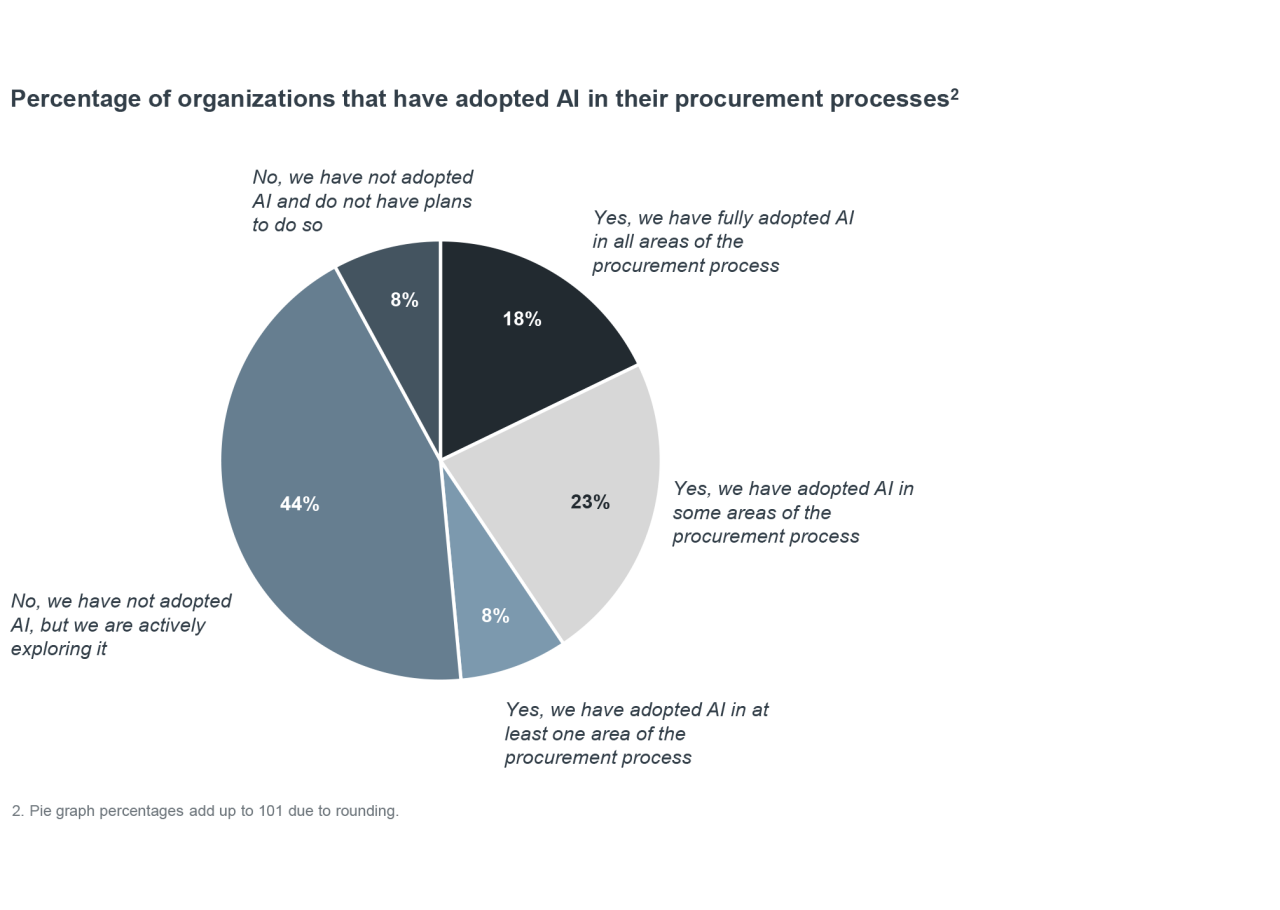
Nearly half of health systems have already adopted AI in procurement, while another 44% are actively exploring its use. That said, only 18% have fully implemented it across procurement functions.
While health systems frequently cite AI as a priority for future investment, many organizations are still in the early stages of adoption. Thus, current efforts are focused less on full deployment and more on foundational work, including establishing governance models, strengthening IT infrastructure, and investing in data assets. Along the way, health systems are prioritizing low‑risk, high‑return use cases that allow them to test these preparations and build confidence before pursuing broader AI transformation.
What’s happening in purchasing today?
Health system leaders view procurement as an ideal area for their businesses to pilot AI tools because existing use cases are relatively simple and low risk from an implementation, governance, and adoption standpoint. As a result, the most common applications in procurement today focus on inventory management and product or vendor identification. These use cases rely on simpler data integration, limit AI’s direct influence over patient care, and allow organizations to demonstrate value quickly while managing risk.
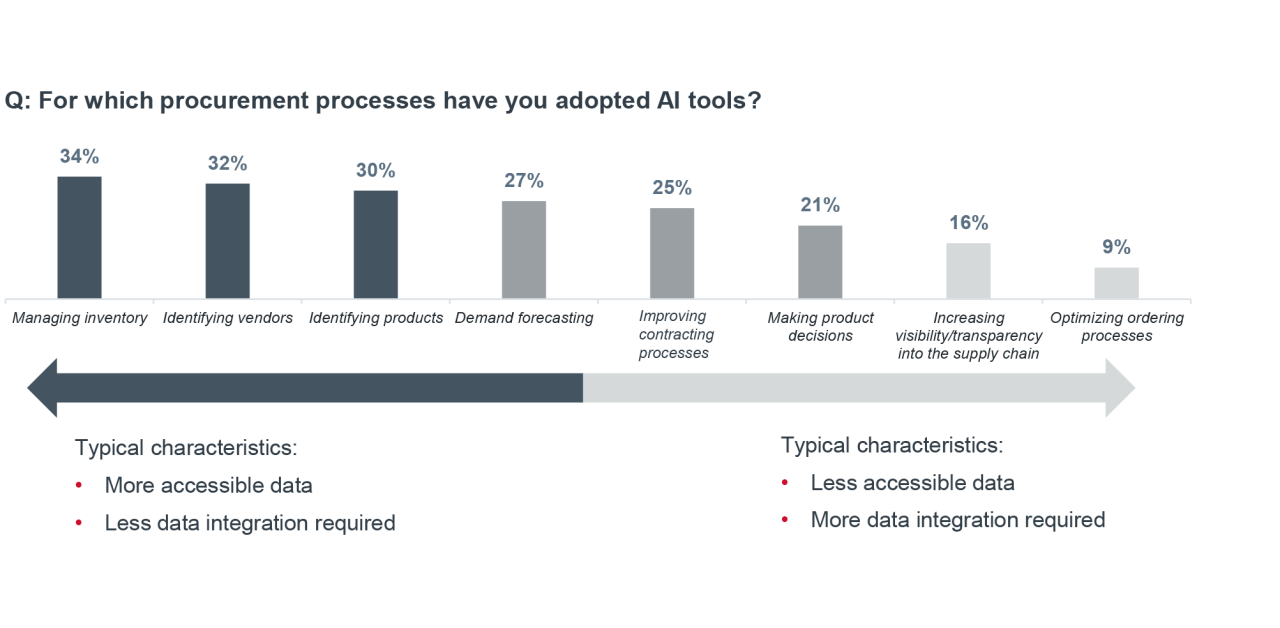
As organizations strengthen data governance and modernize infrastructure, the next wave of AI in purchasing is poised to move beyond basic visibility and into decision support. Leaders are particularly focused on tools that can:
- Leverage demand signals to streamline contracting and ordering, improving speed and accuracy while reducing manual effort
- Inform product purchasing decisions by analyzing product value and comparing options across vendors
- Detect upstream disruptions early and recommend real‑time responses that protect supply continuity
"If you can harness and distill metadata into something meaningful, your teams can make smarter sourcing decisions and frame terms and conditions better."
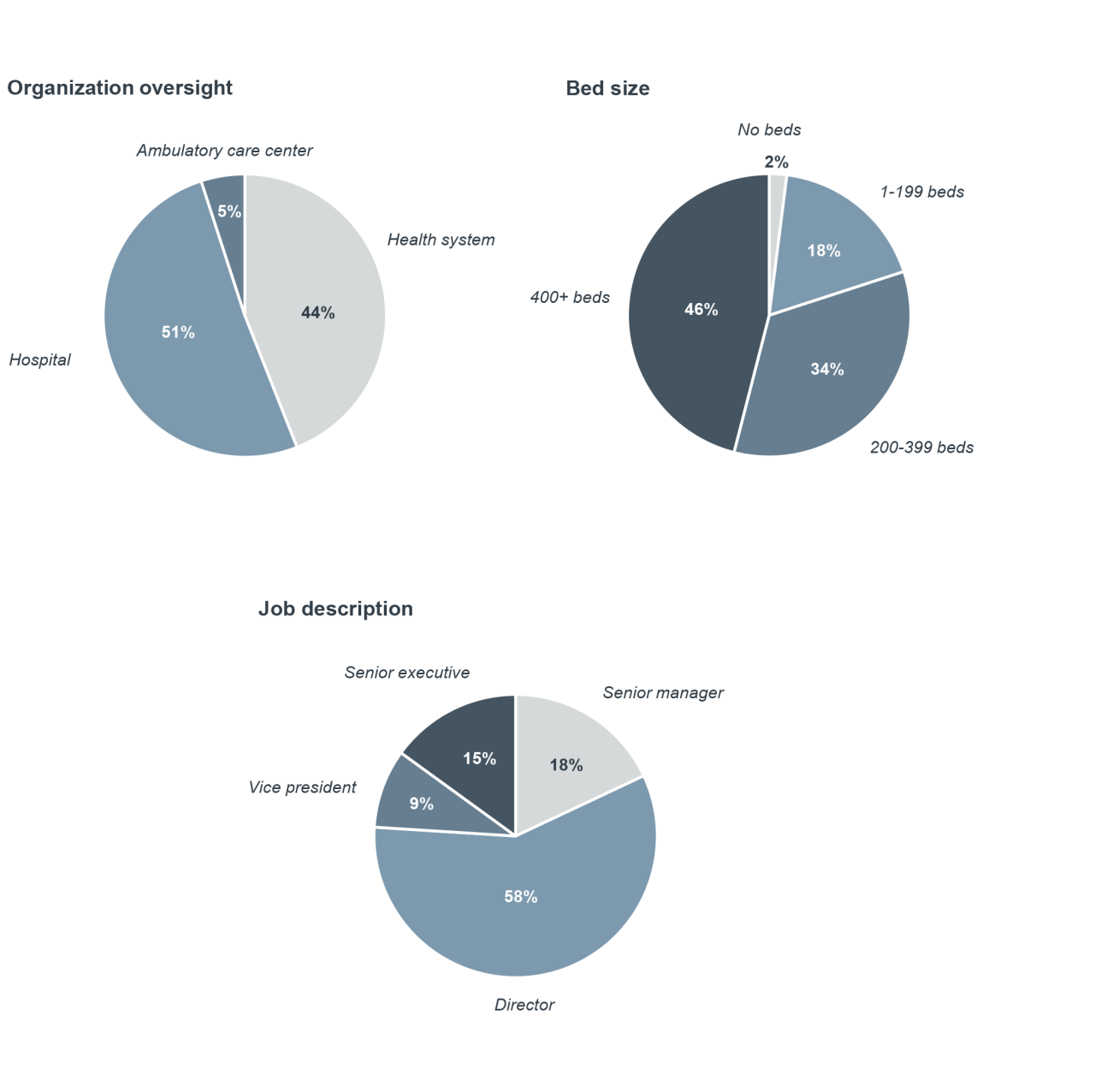
Survey respondent demographics
In 2026, we surveyed 102 health system supply chain and executive leaders across the United States. All respondents play a direct role in procurement decision‑making within their organizations and are responsible for purchases that support day‑to‑day operations. Their perspectives provide insight into the challenges healthcare organizations face today, as well as the priorities, goals, and strategies supply chain leaders use to drive performance and support long‑term success.
As healthcare supply chain leaders face rising costs and margin pressure, they need more than products — they need a partner that drives measurable value. Staples Business helps organizations standardize purchasing and processes, improve visibility, and reduce total cost of ownership with reliable fulfillment, accurate order management, and next-day delivery to over 98% of the U.S.
As a complete non-clinical solutions partner, we provide furniture, EVS, breakroom, print, marketing, and tech, enabling vendor consolidation and simpler indirect spend management. Through data-driven insights and demand management strategies, we help forecast usage, reduce variation, optimize inventory, and prevent overstocking. SKU rationalization and sustainable packaging solutions further help control costs and strengthen supply chain resilience, so health systems can stay focused on delivering exceptional patient care. Learn more here.
This report is sponsored by Staples, an Advisory Board member organization. Representatives of Staples helped select the topics and issues addressed. Advisory Board experts wrote the report, maintained final editorial approval, and conducted the underlying research independently and objectively. Advisory Board does not endorse any company, organization, product or brand mentioned herein.
To learn more, view our editorial guidelines.

This report is sponsored by Staples. Advisory Board experts conducted the underlying research independently and objectively.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.