Auto logout in seconds.
Continue Logout
- Incidental pulmonary nodules are abnormal growths in the lung that are found unintentionally and unrelated to the condition that prompted the exam
- Proper management of IPNs may serve as another tool to detect lung cancer, which is particularly important as lung cancer screening rates remain low
- Without consistent guidelines in place, patients with IPNs may not receive necessary follow-up care. Provider organizations should develop a comprehensive and standardized process to identify, document, and follow up on IPNs
Incidental findings are abnormalities uncovered unintentionally and often unrelated to the condition that prompted an exam.
Pulmonary nodules are abnormal growths that form in a lung. They can be identified on imaging scans, such as X-ray and CT1 scans. Most pulmonary nodules are benign, but some can indicate the presence of lung cancer.
Appropriate detection and follow-up of incidental pulmonary nodule findings may:
- Improve patient outcomes
- Reduce cost of care
- Manage patients’ risk profiles
- Increase appropriateness of care
In 2021, lung cancer was the leading cause of cancer death for men and women in the US. That same year an estimated 12% of all new cancer cases were lung cancer. From 2011-2017, the average five-year survival rate for patients diagnosed with lung cancer was just 22%.
Early lung cancer detection may reduce mortality rates in eligible screening patients by up to 13% – however, only 14% of eligible patients receive the screening exam. Additionally, only patients over 50 years old with significant smoking histories are eligible for the screening exam. While smoking remains the highest risk factor for lung cancer, about 12% of Americans diagnosed with lung cancer have never smoked.
Incidental pulmonary nodule findings may allow more patients with lung cancer to be diagnosed at earlier stages. Detecting lung cancer at an early stage may improve prognosis. But significant barriers exist for proper management, including:
- Providers inconsistently document findings and recommended patient followup
- Communication break downs between providers, such as radiologists and the ordering physician, or between providers and patients themselves
- Patients struggle to understand the findings and their follow-up care needs
- Provider organizations rely on onerous follow-up procedures that confuse patients and their primary care providers
Due to these challenges, patients with lung nodules may fall through the cracks and not receive necessary care.
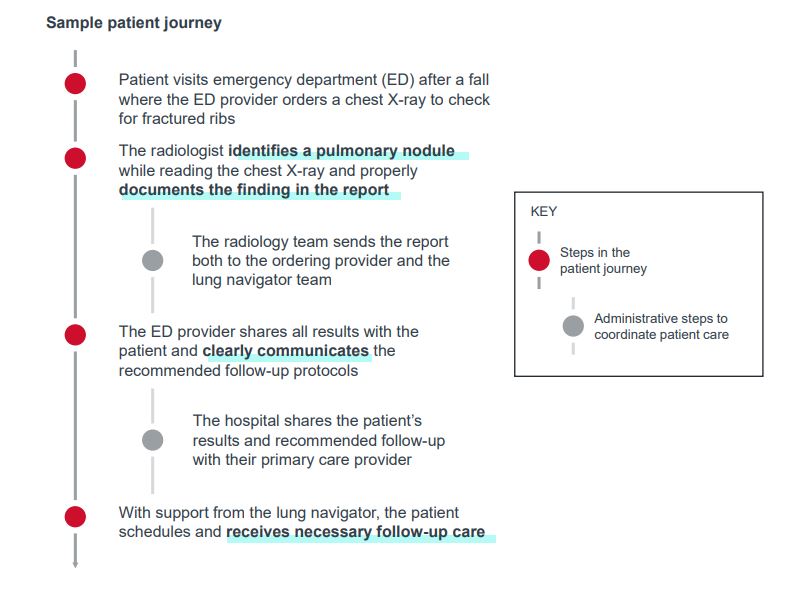
Widely accepted guidelines, such as those from the Fleischner Society or American College of Radiology, detail appropriate clinical management of individual patients. Overall, incidental pulmonary nodule findings and management include three core components:
Identification and documentation
According to the Fleischner Society guidelines, the size and shape of a pulmonary nodule are the two primary determinants of cancer risk. Once a nodule that meets the minimum requirements is identified, interpreting providers, often radiologists, should document abnormalities in a consistent way within reports standardized across the organization. Organizations may leverage artificial intelligence (AI) in imaging interpretation to aid in pulmonary nodule detection and documentation. For example, AI can detect lung nodules on the image and propose a recommendation for a radiologist to reject or validate. Additionally, tools exist to auto-populate follow up recommendations based on clinical guidelines.
Communication
These abnormalities should then be reported to the ordering provider with clear recommendations for patient’s next steps. The ordering provider should then clearly communicate those findings and the appropriate next steps with the patient. The ordering provider and/or radiologist may also discuss the findings with the patient’s primary provider to help ensure follow up or create a care plan.
Follow-up care
Once the patient is notified of their pulmonary nodule, their providers should ensure they receive appropriate follow up. Physicians fail to follow-up on as many as 36% of radiology reports. In order to mitigate gaps, organizations should assign ownership of follow up responsibilities. Many organizations employ navigators who serve a critical role in supporting patient follow up, for example:
- Documenting and tracking patients with incidental pulmonary nodules
- Assisting the patient with administrative functions like scheduling
- Explaining clinical terminology to patients and their care givers
- Communicating with all relevant providers
- Tracking follow-up care and outcomes
Conversations you should considerhaving within your organization
What is our process to consistently identify and document incidental pulmonary nodules? How can we further standardize these guidelines?
How do we educate all providers on the guidelines, processes, and importance of incidental pulmonary nodule findings and management?
What procedures do we have in place for ensuring patient follow up? Where may patients fall through the cracks?
What data do we track related to incidental pulmonary nodule findings and follow up? How can we improve our performance on these metrics?
In partnership with the Lung Ambition Alliance
The Lung Ambition Alliance, a global coalition with partners across disciplines in over 50 countries, was formed to combat lung cancer through accelerating innovation and driving forward meaningful improvements for people with lung cancer. We do this by advocating for improved approaches in three areas: screening and early diagnosis, accelerated delivery of innovative medicine, and improved quality care.
This report is sponsored by AstraZeneca, an Advisory Board member organization. Representatives of AstraZeneca helped select the topics and issues addressed. Advisory Board experts wrote the report, maintained final editorial approval, and conducted the underlying research independently and objectively. Advisory Board does not endorse any company, organization, product or brand mentioned herein

This report is sponsored by AstraZeneca, in partnership with The Lung Ambition Alliance. Advisory Board experts wrote the report, conducting the underlying research independently and objectively. AstraZeneca had the opportunity to review the report.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
