Auto logout in seconds.
Continue LogoutVariation in post-discharge quality and costs, as well as related readmissions, makes post-acute care critical to managing an effective episode of care.
Correct post-discharge patient placement is essential in driving a high quality and cost-effective post-acute episode.
Through primary research and literature review, the Post-Acute Care Collaborative has created a two-part briefing that outlines how health systems can prepare for an efficient discharge process. Correct post-discharge patient placement is critical.
Learn what else you should consider to promote an optimal discharge by downloading part one of our complete guide on the 10 Keys to an Efficient Post-Acute Episode.
Placing patients in the appropriate post-acute care (PAC) setting is no easy task. There’s a wide range of post-acute care settings, and there’s limited standardization around appropriate patient placement criteria for each PAC provider.
Even within providers of the same setting, specialized capabilities can vary significantly. For example, only some SNF providers may be able to care for patients on ventilators. This lack of standardization creates a confusing environment for discharge planners to determine the best post‑acute options for a given patient.
“Currently, there is no standardized process for placing each patient in the appropriate PAC setting. Patients with the same acute-care hospital discharge diagnosis may be referred to different PAC settings. For example, patients who have undergone joint replacement surgery may be treated at a SNF, IRF, or HHA after discharge from the hospital.”-AHA Trendwatch
The risks from inappropriate placement are high. The longer it takes a discharge planner to determine the right setting, the more unnecessary time the patient spends in a hospital bed. At the same time, patients placed in settings that are unequipped to care for them may end up returning to the hospital, while patients placed in unnecessarily high-acuity settings can drive up costs. One study found that between 14% and 42% of post-acute patients, depending on the setting, could be treated in a lower-cost environment.
Proportion of Medicare Patients Place in an Avoidably High-Cost Setting
Study Findings by Post-Acute Setting
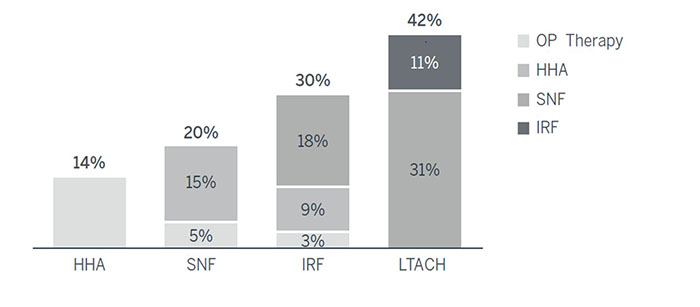
It’s no surprise, then, that bundled payment participants’ post-acute care patterns emphasize utilization of lower-cost settings—notably the home environment.
Get post-acute care resources like this delivered straight to your inbox. Subscribe now
How can you facilitate easy and accurate post-discharge placement of your patients?
Implement a post-acute level-of-care decision guide.
A level-of-care decision guide is a set of criteria mapping specific clinical parameters to the post-acute sectors generally equipped to care for these patients. Case management teams can create their own guide, or select an existing guide such as Interqual® in partnership with referring clinicians.
Work with PAC partners to create a database of contacts and capabilities.
Given the variation in individual providers’ capabilities, discharge planners should also collaborate with local PAC partners to develop a centralized information database with regularly updated information on each PAC partner’s capabilities and a phone number for 24/7 contact. This enables discharge planners to tell at a glance which PAC providers can meet a patient’s needs.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.

