Auto logout in seconds.
Continue LogoutBy Marisa Deline, Practice Manager and Anne Herleth, Senior Consultant, Nursing Executive Center
Last week, we attended the American Association of Nursing Executives' Annual Meeting in San Diego and had the pleasure of speaking with many Advisory Board members and nursing leaders from around the country. The experience also helps us keep a pulse on what nursing leaders care about today—and what likely faces them in the year ahead. Here's our four main takeaways:
Webconference: How you can make every week 'Nurses Week'—and recognize nurses year-round
1. AONE is rebranding—reflecting a shift toward a broader picture of leadership
What was said: The organization, formerly the American Association of Nursing Executives, is changing its name to the American Association for Nursing Leadership. Presenters said the change would reflect the existing diversity within the organization—supporting leaders at all levels and not just focusing on executives. They also want to reflect the organization's focus on building future leaders.
Our take: The new branding reflects much of what we're heaving in our recent calls with members. We're in the midst of setting our research priorities for the year ahead, and more than half of the chief nursing officers (CNOs) we've interviewed have mentioned either addressing nurse leader overload or leadership development needs among their top three priorities. It makes sense; nursing leaders at all levels are critical to the success of the organization, but scoping their roles to be sustainable continues to be a challenge. Here are five strategies we've identified to take on this task and reduce manager overload.
2. Many are concerned about nurse shortages—but it's more about experience than numbers
What was said: There was a major focus on trying to address two evergreen nursing challenges: safe staffing ratios and having enough staff in general. Many hospitals are dealing not with an overall nurse shortage, but with a shortage in experience. As more experienced nurses retire, the workforce is becoming increasingly novice. For instance, one presenting organization predicted three years ago that, if they did not make a change in their workforce planning, 70% of their staff would have less than two years' experience by 2021.
At the same time, care complexity is rising and shows no signs of abating. What this means is that it's not only getting harder to deliver safe care, but there also aren't enough experienced nurses to do it. We see this trend all over the country, so it wasn't surprising that it was a major topic at AONE, and that these conversations quickly shifted into commentaries about acuity, staffing models, the future workforce, and how to deliver complex care without experienced recruits.
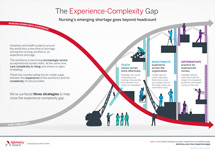
Our take: As leaders grapple with these complex, yet evergreen topics, one thing is clear—the solution has to go beyond just thinking about the number of staff. It's not about nurse-to-patient ratios. It's not about recruiting more staff. It's about how to deliver care to a highly acute patient today, with the staff that hospitals already have. We recently published an infographic on the topic with three strategies to help close this experience-complexity gap.
3. Hospital violence is top-of-mind (and for good reason)
What was said: The uptick in violence against health care workers is well-documented, and, given the number of sessions and posters at the conference that focused on the issue, it's clearly top-of-mind for nursing leaders. Organizations are taking action, with many increasing security budgets to cover more security personnel or install metal detectors. Leaders also talked about how their organizations are looking at addressing the issue in other ways—from tougher state legislation (such as, increasing assault against a health care worker to a felony), to implementing new organizational policies, to organizational risk assignments and new building security.
Our take: Of course, focusing on this extra security is important. But are we thinking about this in the right way? The bulk of violence against health care workers isn't in the hallway—it's at the point-of-care when security isn’t around. The challenge with addressing point-of-care violence is that it's a multi-faceted issue and there isn't one solution that will solve the entire problem. But organizations take a big step in the right direction by equipping nurses to better handle point-of-care safety threats—helping them stay safer and feel safer while at work. To learn more about how, read section one of our report, Rebuild the Foundation for a Resilient Workforce.
4. Technological solutions abound—but leaders need to be smart about which ones they pick
What was said: There continues to be a proliferation of technologies in health care—and nursing leaders are prime targets for their marketing. There were a plethora of technology vendors at the conference, and a variety of sessions highlighting impressive results achieved by using these new technologies.
Our take: Most CNOs and other senior hospitals leaders are bombarded by vendors interested in selling them new products. Many of these products have immense potential. But no organization can afford to buy them all at once, nor do clinicians have the time to learn how to use 10 new technological tools at the same time. That's why it's imperative for nursing executives to partner with other senior leaders in identifying technologies that will help them solve critical business challenges. This requires working from the outside-in, rather than being tempted by what's 'shiny and new' in the technology space.
Here are six key questions we'd suggest asking of any new technology:
- What is the technology, in plain and clear terms?
- How is it disrupting the delivery of care?
- How quickly or slowly should we embrace it?
- How is the innovation leveraged for greater efficiency and efficacy?
- What are the impacts of the innovation on provider financial sustainability?
- How does the innovation support staff engagement and patient experience?
What are you most interested in learning about in the year ahead? Help us set our nursing research priorities in 2019 and beyond by taking our 10-minute survey.
And make sure you register for our upcoming webconference on June 19th to learn more about how you can make every week 'Nurses Week,' and recognize nurses year-round.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.