Auto logout in seconds.
Continue LogoutResearchers recently found that on the way to get an MRI, patients drive by an average of six other places where their MRI could have been done at the same level of quality, but at a lower price.
These patients were considering nonemergency, lower-limb, outpatient MRIs—the type of imaging service that is provided at many different facilities and doesn’t require immediate action. In other words, it should be the easiest to shop around for options. But most didn’t.
This is disappointing news for health plans trying to encourage their members to be more discerning in their health care choices.
Why Money Can’t Buy Habits
Plans know that health care decisions are usually complex and emotional. So most plans try to offer one clear indicator: price.
Plans use a variety of money-based methods to signal that some options are better than others. This can be as simple as clarifying the price so members see the difference. Or it can mean changing the benefit structures, so that members who accept narrower networks and more restrictions pay lower premiums. Many plans even offer financial rewards for doing certain tasks, like choosing a preferred PCP.
But the problem is that price is just a single piece of information, at a single point in time. It’s not enough to create a habit of making cost-effective decisions on a regular, consistent basis.
Four Challenges of Price-Based Health Care Shopping
Put simply, health care is a terrible environment for using money to promote a shopping habit:
1. It’s not actually clear what the best choice is. Rather than providing a signal about potential mistakes, price is actually misleading. Exact estimates are hard to come by. When consumers do encounter a price, they often conflate it with quality. And if the price is too big, the signal can backfire and drive members to reduce all of their care indiscriminately.
2. Price is really uncomfortable to talk about in health care. Plans have historically shielded members from price exposure, so most people think of their insurance as all-or-nothing coverage—not something that varies depending on their choices. And the clinicians who most affect and inform care decisions are not able or comfortable with helping them incorporate costs into treatment plans. There’s a general taboo about putting a dollar amount on the care patients will get.
3. Price-based decisions aren’t appealing—so their effects are muted. Interpreting benefit structures and precisely translating them into cost implications is tedious and difficult. As many behavioral economics studies demonstrate, people default to easier options whenever they encounter resistance. Unfortunately for plans, health care is full of easier decision shortcuts—like service experiences, doctor recommendations, and wait times. All things that often supersede cost considerations.
4. Health care decisions are infrequent and inconsistent. Repetition is key to forming habits, but health care needs arise erratically—and are different every time. Most members get billing surprises or unnecessarily choose higher-cost services when they are receiving a health service for the first time, so it’s difficult to help them become experts in that exact decision.
How to Help Members Form a Good Shopping Habit
Most of these barriers aren’t going away any time soon, but employers are starting to demand better health care navigation support from plans, on behalf of their employees. As a result, we see many plans trying to build the shopping habit on the member's behalf.
One first step to a principled habit: build a familiar routine. Oscar Health, based in New York, is using a steps tracking reward program to teach their members that everything they do in health care should start with the plan, who can advise them appropriately.
Uniquely, their app design puts their members’ top personal—not necessarily health care—interests first. Their A-B testing piloted an interface that put insurance benefits first in one version (A) and steps tracking progress first in the other (B).
Oscar's A|B Test for Member Priorities
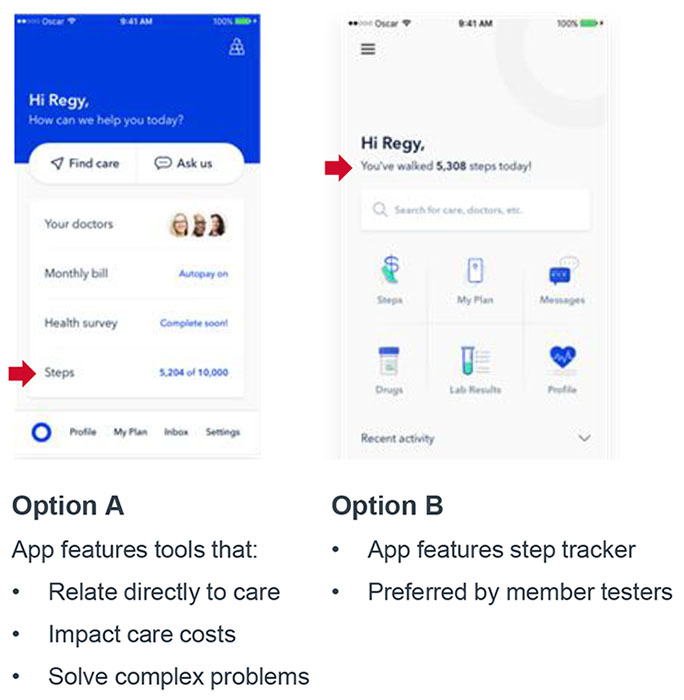
And they found that members preferred a version of the platform that prominently featured the steps tracker at the top when they opened the app, rather than a navigation support tool like a doctor finder.
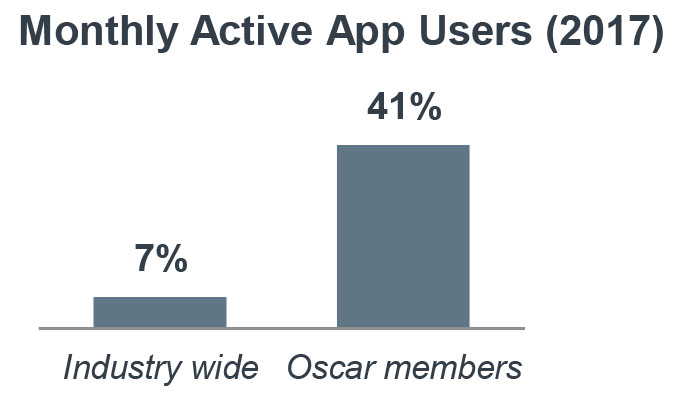
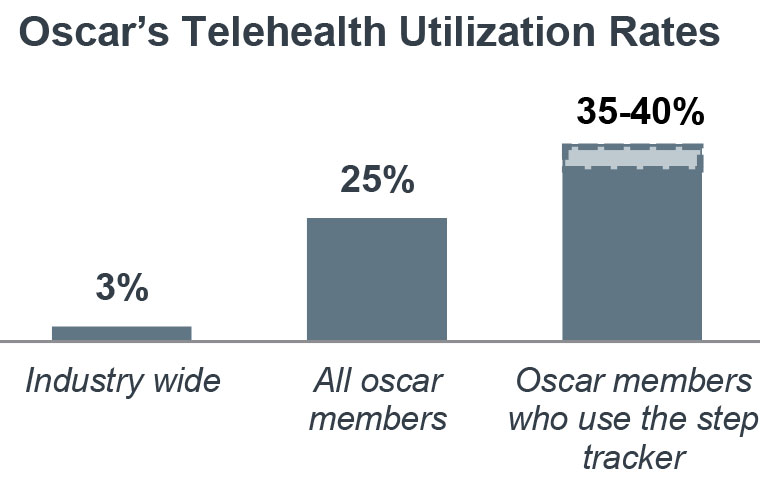
After rolling this out for all members, Oscar drove their engagement rates up by 34 percentage points above the industry average. And this interaction leads to more proactive member engagement in their health care, with Oscar members using the step tracking feature becoming more likely to also use the app for other cost-effective services like telehealth.
Oscar's App Utilization Results
Looking for more strategies to help members make more cost-effective consumer decisions?
Check out our research brief, How to Influence Where Members Seek Care.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.

