The challenge
Healthcare is facing a mounting workforce crisis as administrative and cognitive burdens, physician burnout, and workforce shortages continue to rise.
Clinicians spend more time documenting care than delivering it, spending up to two hours on administrative tasks for each hour of care provided. As the aging population grows, patients no longer present with one or two isolated issues. They have multiple interrelated problems, which require clinicians to remember complex details that increase their cognitive burden. Clinicians simply don’t have enough time in the day to provide and document care and are forced to disrupt their work-life balance by taking work home and completing it after hours.
These mounting pressures on clinicians have led to higher rates of turnover and subsequent gaps in care, which can have a negative impact on patient safety and patient experience.
Through quarterly burnout surveys, University of Michigan Health-West (UMHW) leaders noticed that administrative burden and burnout were becoming more widespread among their clinicians. In post-survey conversations, clinicians relayed that documentation and in-basket messaging were the primary drivers of burnout.
The organizations
University of Michigan Health-West (UMHW) is a nonprofit, multispecialty medical provider based in Wyoming, Michigan. They serve more than 250,000 patients and 61,500 emergency patients through their 208-bed acute-care osteopathic teaching hospital and 30 neighborhood outpatient centers and offices. UMHW has 3,200 employees, including 500 physicians and 700 nurses.
Nuance Communications, a Microsoft company, is a technology pioneer with market leadership in conversational, ambient, and generative AI. They are a fullservice partner trusted by 77 percent of U.S. hospitals and more than 75 percent of the Fortune 100 companies worldwide. Nuance creates intuitive solutions that amplify clinicians’ ability to help others.
The approach
UMHW leaders knew that to improve clinician well-being and support a sustained and fulfilled workforce, they would need to address documentation burden, the chief complaint among their clinicians.
They sought a solution and were intrigued by the promise of AI to address clinician satisfaction, work-life balance, and feelings of fulfillment in addition to achieving a return on investment (ROI). The requirements on their list were that the solution would:
- Enhance the clinician experience by reducing administrative burden, cognitive load, and burnout.
- Help clinicians better treat highly complex patients.
- Improve clinician-patient relationships and patient care.
- Reduce administrative costs through more efficient and effective documentation methods.
- Increase revenue over time.
Leadership at UMHW learned about Nuance’s Dragon Ambient eXperience (DAX) at a conference and selected it as their solution after confirming it met their requirements. DAX is an AI-powered solution that securely records patient-clinician conversations via a mobile application and automatically converts them into clinical documentation. The solution is available for ambulatory specialties, primary care, and urgent care in office and telehealth settings.
The result
UMHW measured the impact of DAX on their organization after using it for over a year. They conducted a study with 83 primary care clinicians that included both qualitative and quantitative research methodologies.
The study revealed that clinicians who used DAX more than 60% of the time:
- Experienced less burnout, with lower rates of exhaustion and disengagement. The drop in burnout after using DAX is comparable to a clinician going from full-time work to part-time work.
- Saw an additional 12 patients per month on average and increased their work Relative Value Units (wRVUs) by 20 per month.
- Found that the revenue generated from the additional visits covered the cost of DAX with an additional 80% return on investment.
How UMHW used DAX to reduce documentation and cognitive burden and increase throughput
UMHW was thoughtful about the requirements for measuring success. The following approach helped them implement and scale DAX to promote clinician well-being, reduce documentation burden, and increase patient throughput.
The three elements
Clinician well-being is a priority at UMHW — one that all their leaders are deeply committed to — which enabled widespread buy-in of the solution. Leaders understood that DAX would eliminate what UMHW considers to be the hardest 90% of a clinician’s job — documentation. Reducing that burden alone would decrease burnout, improve clinician morale, and promote the organization’s commitment to their clinicians.
This mindset drove clinician adoption because they recognized DAX as a solution meant to work for them. UMHW leaders were very clear that DAX’s primary purpose was not to force clinicians to increase the number of patients they should see or take on more work. Instead, leaders believed that improved well-being would benefit clinicians and naturally result in increased productivity and financial returns for the organization.
We can’t go at this with the mindset that providers can see more patients. They will be able to, but they just don’t believe it before they use DAX. We must think in the way that we are improving the experience for both providers and patients. With this, the entire industry benefits. The soft ROIs are almost immediate, the hard ROI will come after the investment.
Clinicians were excited about a solution that would relieve their documentation and cognitive burden, help them get home on time, and prioritize personal interests outside of work. Many UMHW clinicians recognized the potential for DAX to improve their quality of life right away.
Clinicians were excited about a solution that would relieve their documentation and cognitive burden, help them get home on time, and prioritize personal interests outside of work. Many UMHW clinicians recognized the potential for DAX to improve their quality of life right away.
UMHW identified a group of initial users, comprised of primary care clinicians, to try DAX before scaling the solution across their entire primary care program. UMHW found that these clinicians were well suited to DAX for two reasons:
- Primary care has seen an increase in complex, less “templated” visits.
- UMHW’s primary care clinicians demonstrated an openness to technology.
Primary care has seen an increase in complex, less “templated” visits.
Primary care clinicians at UMHW see many patients with complex illnesses, and whose health information can’t easily be documented in standard note templates in the EHR. UMHW’s clinicians have always treated patients with multiple issues, but it’s becoming even more common to see these patient types. For example, patients increasingly come to their annual visits with a list of many unrelated issues to discuss. Standard note templates aren’t designed to gather information for matters outside of the standard annual visit, so clinicians must take the time to manually fit this information into the note. The typical visit isn’t long enough to capture the added complexity, so clinicians must finish notes between visits or at the end of the day. This requires them to remember each patient’s specific details for hours and increases the risk that clinicians will forget key information by the time they’re able to complete a note.
UMHW found that their primary care clinicians were eager to use DAX for patients with complex needs. DAX securely records conversations in real time, which eliminates the potential to forget or miss key details. The solution also eliminates the need to use a template because it creates a structured note on its own. Even clinicians who were initially hesitant gave DAX a chance because they saw how it alleviated documentation burden.
UMHW’s primary care clinicians demonstrated an openness to technology
UMHW has worked hard to promote innovation among its staff, and their primary care clinicians embody that philosophy. They use a top-down approach with clinician leaders who model how to be comfortable embracing change and approaching new technology. The result is that many of UMHW’s primary care clinicians were willing to start using DAX because they self-identify as “technologists” and “early adopters.”
Primary care is often overlooked and underinvested in when it comes to new technology for a variety of financial and logistical reasons. Knowing this specialty hasn’t always been at the forefront of new investments, UMHW was intentional about offering DAX to their primary care clinicians first to include them in their culture of innovation. They found that these clinicians were genuinely excited and appreciative of the opportunity to test a new way of documenting care.
After initial success, UMHW expanded DAX across their entire primary care service line. Due to the overwhelming success, UMHW decided to expand the program to all ambulatory specialties.
UMHW found that DAX was relatively quick and easy to implement. The onboarding process was simply a one-hour training for all users. UMHW leaders said that the hardest part of onboarding was finding a free hour in clinicians’ busy schedules to do the training.
DAX was the easiest project to launch, with the largest impact, in my career.
UMHW acknowledged that there’s a period of adjustment as clinicians go through the learning curve and adapt to changes in their routine. Even among innovative organizations, change is hard, and that’s especially true for clinicians who are often set in their ways.
To help with adoption, UMHW enlisted provider champions, such as Dr. Lance Owens, CMIO of UMHW, to frequently check in with clinicians and aid them through the adoption process.
Sharing key performance indicators (KPIs) was also key to adoption. Instead of forcing clinicians to use DAX, UMHW shared KPIs from their initial DAX cohort, which included information on documentation time saved, to help them see how they could achieve the same results with consistent use.
Clinicians realized three improvements when they started using DAX consistently:
- DAX freed up clinicians’ time and decreased cognitive load.
- Patient care improved and billing was more complete due to the increased detail and structure of the notes.
- The use of DAX strengthened patient relationships by allowing more focus on the patient and no distractions with note taking.
DAX freed up clinicians’ time and decreased cognitive load
Clinicians found that DAX drastically improved workflows and their cognitive burden by automating clinical documentation.
Clinicians don’t have to manually type notes or stress about documenting after hours when they use DAX. They also don’t have to struggle to remember details from the visit since they could refer to the transcript. As a result, clinicians were able to give patients their full attention during a visit and focus on other clinical tasks, like coordinating with members of their care teams between visits.
There was a point where I had to slow down my schedule because the cognitive burden was so high. But with DAX, there’s less cognitive burden so I can see more patients without feeling burned out.
Patient care improved and billing was more complete due to the increased detail and structure of the notes
Clinicians found that the notes generated by DAX were more comprehensive and at times phrased differently than the notes they would manually create. In the beginning, clinicians spent time reviewing their notes to check the information and adjust the note to their own preferences. The review process became faster the more clinicians used DAX.
Clinicians came to appreciate the level of detail in the DAX-generated notes, recognizing DAX included information that clinicians either didn’t have time to capture, or would have left out if they were manually typing notes. This leads to better patient care since clinicians have a more accurate record of what occurred during a visit. They can double-check that every lab they said they would order was submitted, or that they didn’t miss anything when explaining treatment plans to patients. Patients can also look at notes to review anything discussed during a visit, such as care instructions or procedural information. This results in retaining patients who feel their clinician was focused on them and creates loyalty with the health system.
DAX notes are more detailed because it’s able to record things that clinicians don’t have the capacity to manually record.
Higher quality notes also enable more accurate billing and improve RVUs. Having a detailed record of everything that occurred during a visit allows clinicians to ensure that the documentation accurately reflects the services rendered.
Notes are more detailed and complete which helps with more accurate billing and helps patients with follow-up care months after a visit.
DAX strengthened patient relationships
Overall, clinicians said that DAX strengthened their relationships with patients. In rare cases, there were patients who had questions about being recorded. In those instances, clinicians would take a few additional minutes at the beginning of the visit to explain how DAX worked and answer any questions.
Clinicians found that patients appreciated having face-to-face conversations, instead of watching clinicians type notes on a computer the entire visit, which strengthened their relationship. Many patients commented on this change directly to their clinicians, saying that they seemed more present, and the interactions were more personal. Patients were also impressed by the “high-tech” nature of the solution, which had a halo effect on their entire care experience.
The atmosphere is more relaxed when I don’t have to worry about documentation. Patients will even say thank you for spending more time with them, even when it’s the standard amount of time — it’s just the perception that we’ve had more time.
UMHW saw improvements in clinician well-being, an increase in productivity, and found that the revenue covered the cost of DAX with an additional 80% return on investment.
It’s important to remember that UMHW leaders prioritized clinician well-being and found that the financial return from increased productivity was a natural byproduct of that commitment.
Anything that can give me more family time and time with my kids is worth it, and DAX does that for me.
Clinicians saw an overall improvement in their satisfaction and well-being
Clinicians reported spending less time documenting care, which allowed them to go home at a reasonable hour without bringing work with them. The time spent documenting was reallocated to things that clinicians previously rushed to complete between visits, like interpreting lab results or preparing for cases with their care team.
DAX has brought a real sense of work-life balance to caregiving. I can naturally keep up with notes and still have time to do other things.
UMHW provider survey shows lower burnout among high utilizers of DAX
UMHW conducted provider burnout surveys in April 2023 to measure the impact of DAX on clinician burnout. Eighty-three clinicians that had been using DAX for at least a year took the survey. Blinded data on the percentage of encounters conducted with DAX was used to determine if a clinician was a high or low utilizer.
The clinicians that used DAX were also asked to complete the Oldenburg Inventory (OBI), which measures burnout on a scale of 64, with 1 being the lowest level of burnout and 64 being the highest level of burnout.
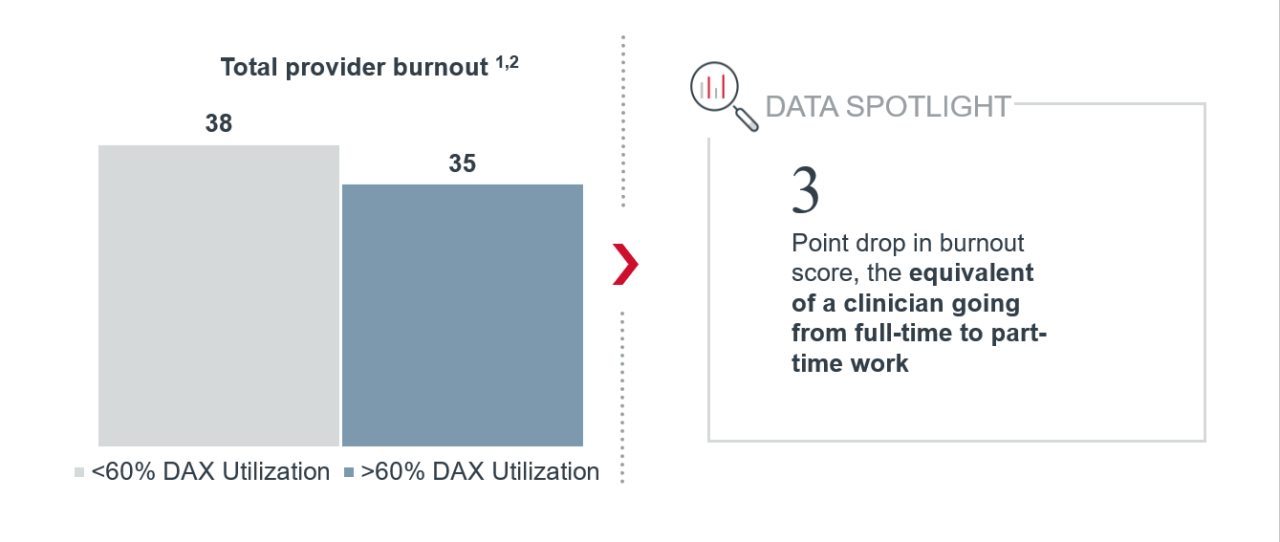
The results showed that the highest utilizers of DAX experienced less burnout and disengagement. In fact, there was a three-point decrease in burnout rates between clinicians who use DAX more than 60% of the time and clinicians who use DAX less than 60% of the time. That drop in burnout is comparable to a clinician going from full-time work to part-time work. High utilizers of DAX were also less likely to talk about work in a negative way, more likely to have enough energy for leisure activities after work, and more likely to feel engaged and energized at work.
An increase in efficiency and productivity led to financial returns
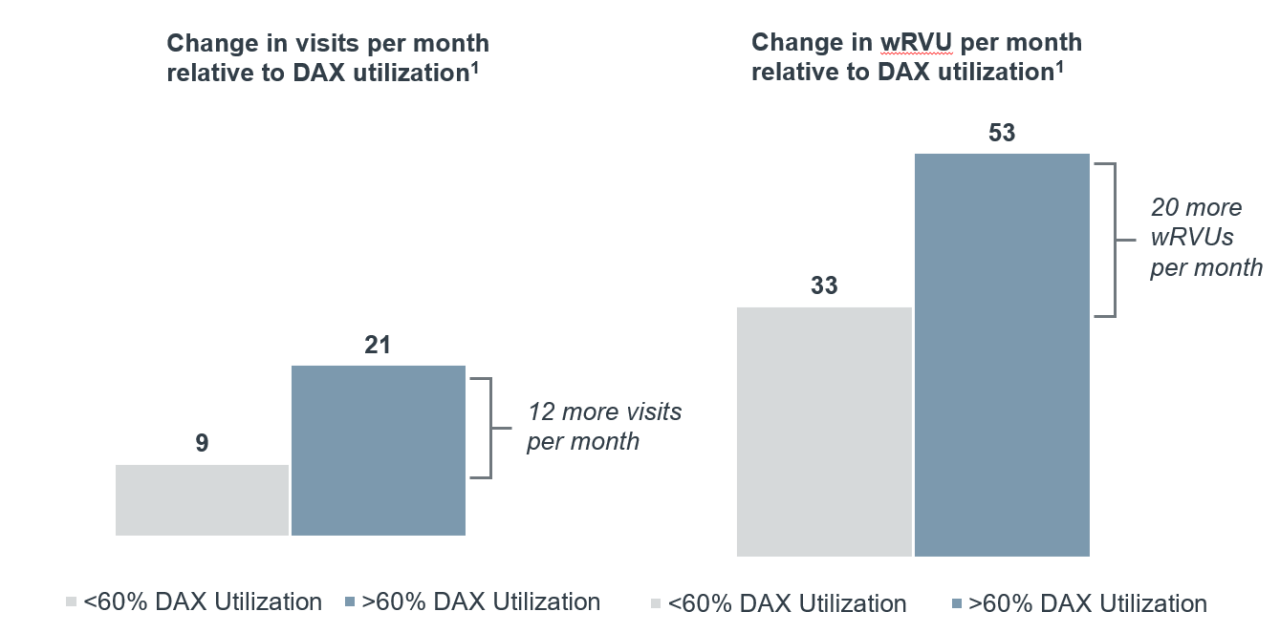
UMHW also measured the increase in visits per month and work RVUs pre- and post-DAX usage. It’s worth noting that the number of hours clinicians are required to see patients was reduced by 4 hours in an effort to further decrease burnout during the post-DAX usage period.
While increasing productivity wasn’t the main driver of DAX for UMHW, their clinicians found they could naturally add visits because of increased efficiencies, even with the contact hour reduction. Clinicians reported that they only needed to allot 15 minutes for a single appointment instead of the standard 30 minutes because they didn’t have to reserve time for documentation.
All clinicians in the cohort increased their number of visits and work RVUs after using DAX. Clinicians that used DAX for more than 60% of their encounters saw an average of additional 12 visits per month and increased their work RVUs by 20 per month compared to those that used it less than 60% of the time.
Nuance Communications is a technology pioneer with market leadership in conversational AI and ambient intelligence. A full-service partner trusted by 77 percent of U.S. hospitals and more than 75 percent of the Fortune 100 companies worldwide, Nuance creates intuitive solutions that amplify people's ability to help others. Nuance is a Microsoft company.
This report is sponsored by Nuance Communications, an Advisory Board member organization. Representatives of Nuance helped select the topics and issues addressed. Advisory Board experts wrote the report, maintained final editorial approval, and conducted the underlying research independently and objectively. Advisory Board does not endorse any company, organization, product or brand mentioned herein.
To learn more, view our editorial guidelines.

This report is sponsored by Nuance Communications. Advisory Board experts wrote the report, conducting the underlying research independently and objectively. Nuance had the opportunity to review the report.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.


