Auto logout in seconds.
Continue Logout- AI is an umbrella term that covers a range of different technologies, each with different types of capabilities and levels of complexity
- AI can enhance a wide range of objectives in health care by improving the cost, speed, accuracy, and consistency of various processes
- AI in health care is not intended to replace human workers and will not always be perfect. Rather, having good data and appropriate human input can bring better results than humans working alone
Artificial Intelligence (AI) is not a single technology, but rather a field of technology able to perform tasks that normally require human intelligence by using algorithms, heuristics, pattern matching, and other techniques within the realm of computer science. AI has been an area of significant interest for the health care industry for several years, and many health systems, payers, and life science organizations have (or plan to) incorporate AI and automation into their business strategy.
AI capabilities can be broken down into Narrow AI and General AI. Virtually every AI solution today uses Narrow AI. Narrow AI algorithms solve a tightly defined task, such as finding pneumonia in an x-ray, or powering a patient portal chatbot, but have limited utility outside the task for which they were designed. General AI is a more adaptable intelligence that can understand context, quickly adapt to new situations, and apply knowledge to a wide variety of domains—but such AI may be technically impossible to achieve.
Below are a few AI-related terms that are useful to distinguish:
- Advanced Analytics: a broad category including AI, predictive analytics, and prescriptive analytics to augment processes and predict future events
- Machine Learning (ML): a range of techniques including strategies like time-series analysis, which allow computers to learn to perform tasks without being explicitly programmed. Uses advanced statistical techniques to identify patterns in data and then make predictions from those patterns with a degree of certainty
- Natural language processing (NLP): techniques which allow computers to understand human language and communicate back with similar language
- Robotic Process Automation (RPA): the use of automated robots to handle repetitive tasks, generally not highly “intelligent”
Not all AI functions have the same degree of intelligence. This statement equation can explain how to determine the extent of a system’s intelligence:
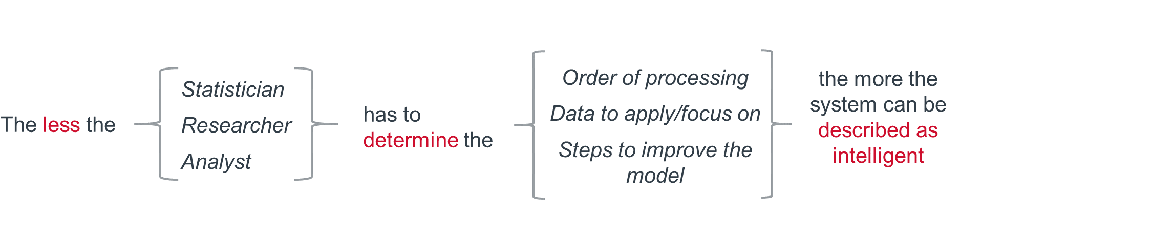
Looking specifically at intelligent functions, it can be helpful to understand types of technologies based on what they do—their abilities and use cases. Below is an example of several types of AI applications, categorized by their functions.
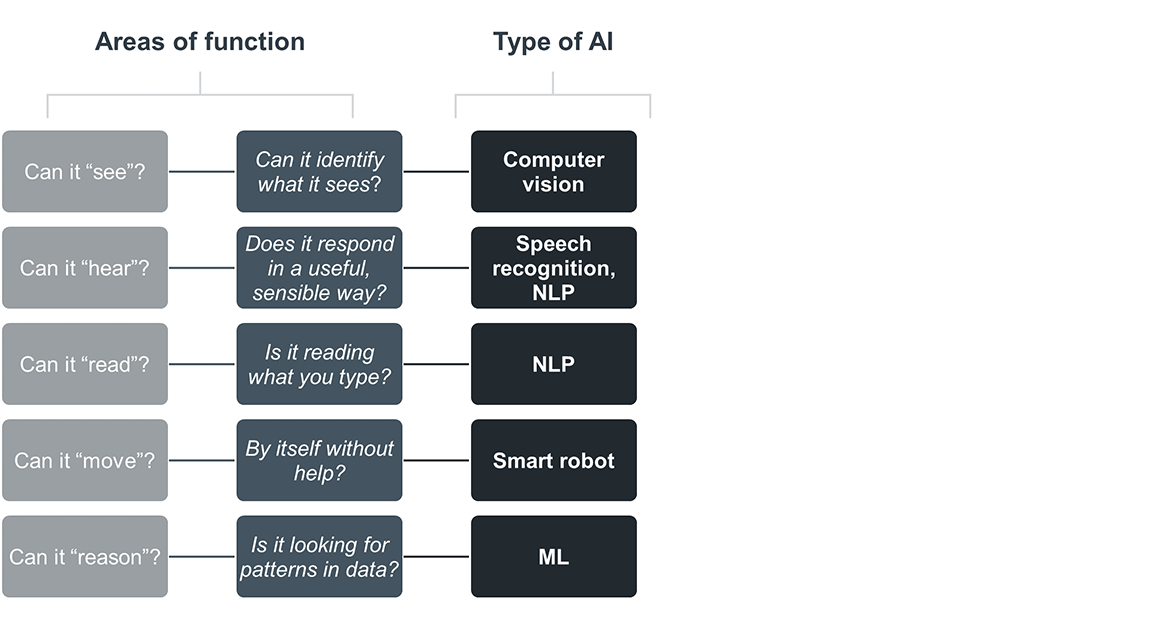
When supplemented with human intelligence and action, the use of AI systems in health care can provide advantages in three key areas:
1. Improves speed, capacity, consistency, and accuracy: Computers don’t forget what they have learned, don’t get tired, and can recognize shifts or patterns in data more quickly and comprehensively than most humans (once they are trained appropriately). Automation and AI can run thousands of tasks at once – something impossible for humans alone to achieve.
2. Addresses the increased amount of data: Health care experts (no matter how experienced) can only take in, comprehend, and act on so much data at one time, and in health care the breadth and depth of data are growing exponentially. AI can help process the rapidly expanding amount of structured and unstructured data from sensors, medical devices, mobile apps, and EHRs to make data more actionable.
3. Enhances the abilities and efforts of human workers: AI can help free human experts from repetitive or tedious tasks, continuously monitor complex situations, discover patterns and anomalies, and ensure that tasks do not fall through the cracks. AI can be a trusted and capable assistant, augmenting human capabilities across the value chain.
With these key benefits in mind, AI can take on a wide range of potential use cases within health care, including research, education and training, clinical decision making, patient engagement, and business operations. Simpler forms of automation such as RPA can handle a variety of rote processes, while more advanced Machine Learning and other “intelligent” functions can greatly improve processes for a variety of both clinical and administrative areas.
AI in health care can encompass a wide variety of products, ranging from robotic process automation (RPA) scripts that assist with financial processing, to NLP that helps physicians record visit notes, to computer vision programs that can improve the accuracy of imaging results.
The level of complexity can range from relatively simple to extremely complicated. However, AI programs are generally designed to fit into existing workflows with the aim of augmentation, not disruption. AI is generally more widespread and established in administrative processes such as revenue cycle management, while AI for clinical purposes such as diagnosis is relatively narrower in potential use cases for now. Below are simple illustrations of how AI can work in different potential settings.
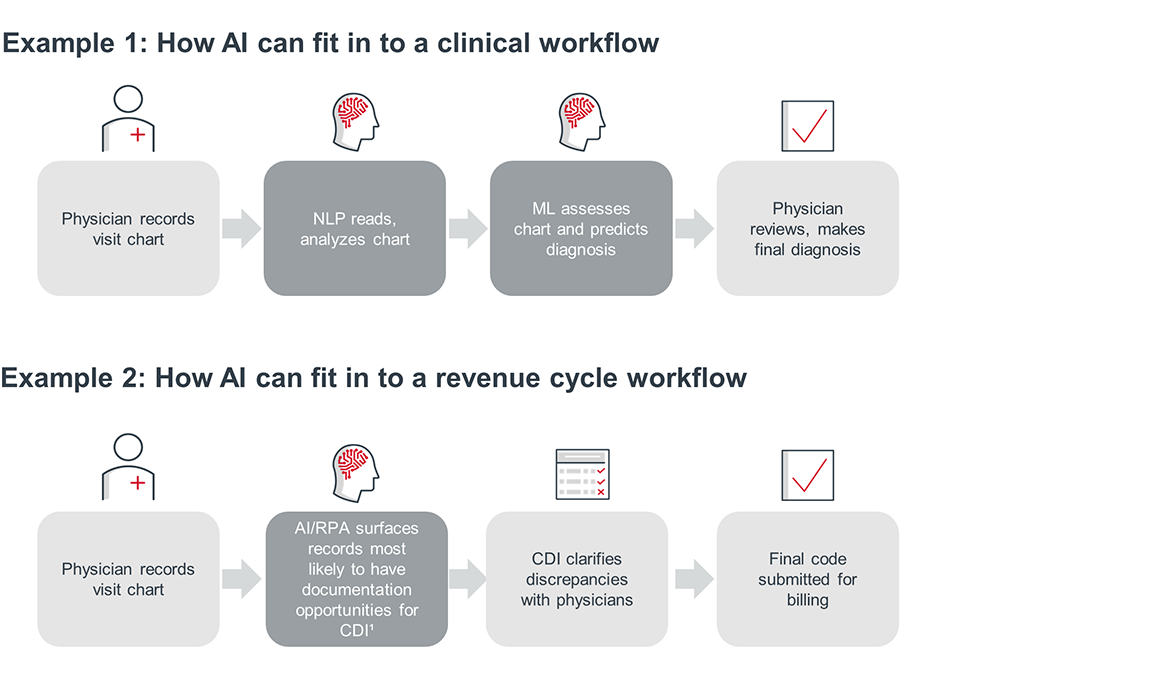
Despite myriad benefits, there is still very serious skepticism about applying AI in health care. In general, there are three primary sources of skepticism that can slow adoption in health care settings:
First is the uncertainty around how AI programs produce their outputs, also known as the commonly-cited “black box problem”. With most AI tools, there is virtually no way to tell how a result is produced. However, developers are creating several “white box” or explainable AI (XAI) models designed to improve transparency around how AI programs work internally.
Another concern is whether AI will replace or “take over” people’s roles. In general, AI solutions are not intended to replace workers wholesale, but rather to support and augment administrative and decision-making processes to reduce extra burden, improve accuracy, and allow workers to practice at top-of-license. AI still works best when paired with human oversight, as systems may not perform predictably when faced with parameters outside of their normal range of experience.
Finally, there are questions around the accuracy and bias of AI outputs. Much like human workers, AI will not produce perfect results every time, because good AI is only possible with good data inputs. Especially for AI that uses population-level inputs, data that is biased or skewed can lead to inaccurate results and worsened heath disparities. AI will succeed when its data inputs are accurate, unbiased, and representative. When AI works alongside human decision-makers and is maintained properly, it can significantly improve speed, cost, capacity, and outcomes for a wide range of processes in health care.
Conversations you should be having
Are there problems in our organization that AI can be useful in solving or mitigating? Which problems are best suited to an AI solution, and which ones aren't?
What attitude do staff in our organization have about AI and automation? Where is there skepticism, and what's driving it? What is our communication plan to promote greater acceptance of AI and automation?
How will our organization ensure that the quality of data inputs are accurate, unbiased, and representative, to ensure that our use of AI does not exacerbate existing inequities?
How will our organization continue to improve and maintain AI over time? What plans do we need to put in place, and who will be accountable for doing so?
In order to make the best use of AI in your organization, it’s important to start with a specific problem or goal you want to solve, rather than with a specific AI you want to implement. Review organizational performance data and speak with top-performing staff about what’s keeping them from making the best use of their time to pinpoint the right opportunities.
Iodine Software is an enterprise AI company that applies groundbreaking machine learning that interprets clinical data to generate highly focused, predictive insights to dramatically advance the effectiveness of patient care professionals and the healthcare enterprise as a whole. Iodine's powerful predictive engine, Cognitive ML, constantly ingests the patient record to generate real-time, clinically-informed, unique predictive insights—facilitating critical decisions, scaling clinical workforces through automation, and improving the financial position of health systems.
Learn more about Iodine Software
This cheat sheet is sponsored by Iodine Software for educational purposes only. The content, views, and opinions contained within the cheat sheet are copyrighted by Advisory Board and all rights are reserved. Advisory Board experts wrote the content, conducting the underlying research independently and objectively. Advisory Board does not endorse any company, organization, product or brand mentioned herein.

This report is sponsored by Iodine Software, an Advisory Board member organization. Representatives of Iodine Software helped select the topics and issues addressed. Advisory Board experts wrote the report, maintained final editorial approval, and conducted the underlying research independently and objectively. Advisory Board does not endorse any company, organization, product or brand mentioned herein.
Learn moreDon't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.

