Auto logout in seconds.
Continue LogoutImproving patient access is key to ensuring patients receive low-cost care in the most appropriate setting. But expanding access requires an investment—often in staff and infrastructure. And with a slew of options including retail clinics, mobile apps, and "hospital at home," determining where to start is not a simple decision.
One way Massachusetts General Hospital is addressing their access challenge is by collaborating with Partners HealthCare at Home (PHH) in deploying nurse practitioners (NPs) to patients' homes, specifically for elderly patients.
Elderly patients seeking care in the ED far too often
Like many health systems, Mass General struggled with an influx of unnecessary ED and hospital visits. To address this problem, leaders targeted their elderly patient population, and with good reason: this population had a high frequency of "precautionary" ED visits. These visits often resulted in hospital admission as an added precaution, despite elderly patients having a heightened risk of contracting serious illness in hospitals.
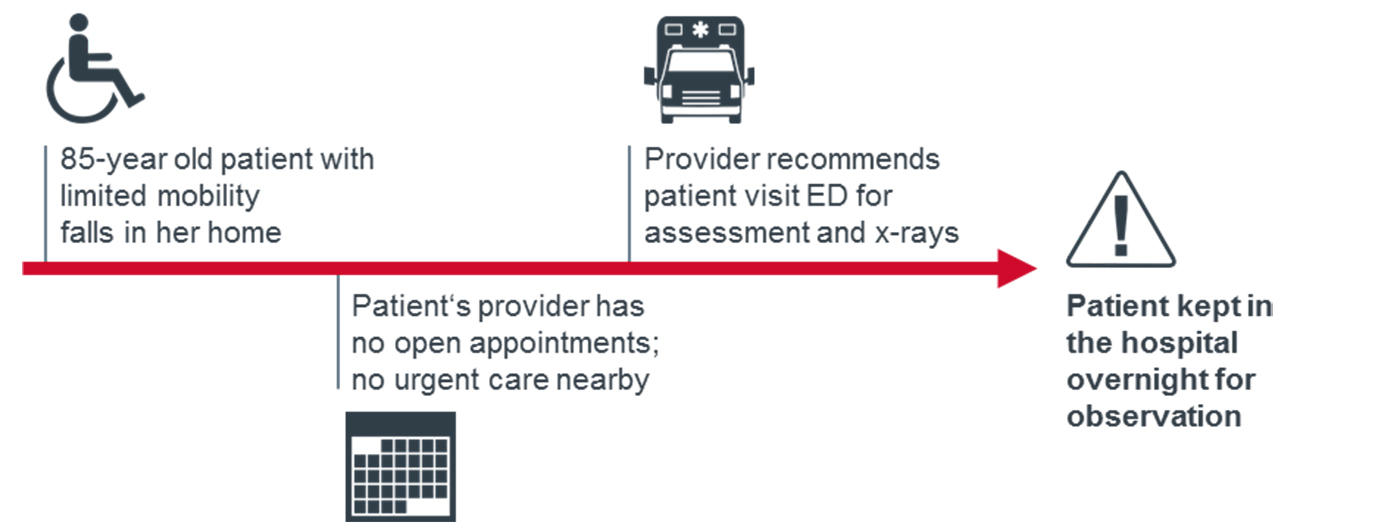
Digging deeper, leaders found that primary care providers, despite their best intentions, were part of the problem. For example, if an elderly patient with limited mobility falls at home, a provider with a fully booked schedule might recommend the patient take a trip to the ED by ambulance. But providers can't be blamed for taking this type of precaution—especially with no alternatives for ensuring patient safety. It became clear to leaders that they needed to design a less costly, patient-centered way for these patients to receive care outside of the ED.
Bringing urgent care services to the patient's doorstep
To reduce unnecessary ED and hospital encounters for elderly patients, leaders at Mass General looked to Partners HealthCare at Home (PHH), who designed a system to bring care directly to patients.
Services provided in the home through doorstep urgent care include:
- X-ray
- Ultrasound
- IV therapeutics
- EKGs
- Blood tests
- Wound treatment debridement
- Dopplers
- Coordination of hospice care, palliative care
- Referrals to occupational therapy, physical therapy
PHH deploys NPs, who each cover a geographic region, to provide urgent care services for patients in their homes. Now, instead of sending a patient to the ED after a fall, a provider can send an NP to the patient's home for an examination. This partnership with a vendor allows patients to even get X-rays in their homes.
PHH and Mass General began their collaboration on this program in the summer of 2015, and they've already seen positive results. Leaders found that 70% of patients who used the service would have otherwise been sent to the ED, and almost half would have been admitted.
If you're considering this strategy for improving access and providing care in a more patient-centered, appropriate setting for your organization, Mass General and PHH found three critical elements for success:
- Provider buy-in. PCPs must be on board and willing to refer their patients to the service.
- The right NPs. This role suits NPs' skill set, but you can't assume a caregiver who wants to provide urgent care services will be interested in the less-traditional aspects of this role, such as driving around a city and going into patients' homes.
- Access to equipment. PHH partners with an external vendor who sends an imaging tech to meet the NP at the patient's home with mobile and hand-held imaging equipment when needed.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
