Auto logout in seconds.
Continue LogoutSome Chicago-area hospitals are testing new "lung in a box" technology that aims to increase the supply of donor lungs by giving previously unusable organs a second chance, Lisa Schencker reports for the Chicago Tribune.
Here are 5 key tactics to attract and retain transplant patients
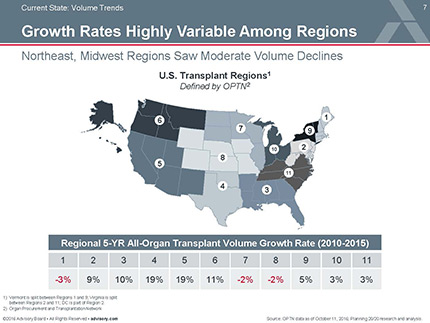
Although fewer people are on the waiting list for lung transplants than for kidneys, livers, or hearts, lungs are the hardest organ to come by, Schencker reports. About 80% of donated lungs are deemed unusable, often because the organ was damaged while a patient was on life support.
Daniel Dilling—medical director of Loyola Medicine's lung transplant program, which is testing the new technology—said that people "unfortunately are dying while waiting for transplants." Dilling said that the "lung in a box" technology is "by definition increasing the pool of donor (lungs) available."
How it works
The technology, officially called ex vivo lung perfusion, allows researchers to extend the life of a lung once it has been removed from the donor's body—giving doctors more time to determine whether an organ is in fact fit for transplant.
Researchers place the donated lung in a transparent dome and connect it to a ventilator that blows air and oxygen into it—much like a scene from a science fiction movie, Schencker writes. The air inflates and deflates the lungs in the same way that breathing does, while a solution of proteins and nutrients are pumped into the vessels of the lung to keep it alive.
Doctors then observe and test the lung for a few hours to determine whether it's healthy enough to be transplanted. In some cases, Schencker writes, the technology can even repair damaged lungs.
Credit: Loyola Medicine
FDA has approved the technology for use in clinical trials, and two hospitals—Loyola and the University of Chicago Medical Center—have separately tested a total of five lungs and transplanted three.
Costly technology
Tae Song, surgical director of the University of Chicago's lung transplant program, said that this technology will expand "our donor pool to lungs that are almost perfect but not quite, to lungs we would have turned down before, and that translates to shorter wait time[s] for patients."
However, some hospitals are hesitant to invest in the technology, which Schencker writes can be very expensive, requires specially trained staff, and is used fairly infrequently.
Ankit Bharat, the lung transplant director at Northwestern Memorial Hospital, said Northwestern has relatively short wait times for transplants and has never had a patients die waiting for a lung transplant. "For us, it didn't make sense to take a marginal lung we would not normally use," Bharat said. He added that the technology is "a significant advancement," but said that "just because it's there doesn't mean that every patient needs it."
Similarly, Christopher Wigfield, surgical director for lung transplantation at Advocate Christ Medical Center in Illinois, said that he considers the technology to be important, but that it could also create a major cost, as not all lungs connected to the technology will ultimately prove usable.
But Dilling said he is hopeful that the clinical trial will prove to be financially beneficial and that more hospitals will be able to use the technology (Schencker, Chicago Tribune, 5/18).
Here are 5 key tactics to attract and retain transplant patients
Download this briefing to learn how to expand the pipeline of potential transplant patients and engage them across the care pathway.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.