Auto logout in seconds.
Continue LogoutRead Advisory Board's take on the growth of the C-suite.
To keep up with an increasingly complex and consumer-driven health care market, health systems are adding non-traditional C-suite positions—and "creating a new picture of just what a hospital administration looks like," Jeff Lagasse writes for Healthcare Finance News.
New roles
According to Lagasse, some increasingly common examples of new C-suite roles include:
- Chief innovation officer (CIO, or CINO), who oversees innovation and change;
- Chief learning officer (CLO), who oversees learning initiatives, staff training, and development to ensure staff effectiveness;
- Chief quality officer (CQO), who oversees quality goals and develops methodologies to achieve them; and
- Chief transformation officer (CTO), who oversees a hospital or health system's efforts to move the organization forward.
Several health care organizations are incorporating these or similar roles and similar ones to drive their growth and meet demand in a consumer-focused market, Lagasse writes. For instance, Northwell Health has added the positions of CLO and CIO, among others, over the past 15 or so years,
What's driving the trend
Northwell EVP and COO Mark Solazzo called the growing C-suite, "a reflection of the market dynamics." He explained, "The health care marketplace has been changing markedly over the past decade, and will continue to change. ... We need to create an organizational structure that can respond to the marketplace changes, whether it's making sure you can compete on the people side of the business, or making sure the organization is in line with regulatory compliance."
Separately, Kathleen Kinslow—former CEO of Aria Health, who currently serves as EVP and chief integration officer for Jefferson Health and CEO of Aria-Jefferson Health—said her role changed based on the integration needs that arose when Jefferson merged with Abington Health in 2015 and with Aria in 2016.
"I think [the new role] highlights a shift in what hospitals hope to achieve when they combine," she said, adding, "For a long time, hospitals sought partners for financial strength and stability, usually during a time of financial challenge. More recently, leaders of health systems are looking for combinations that deliver significant, strategic long-term benefits. ... Gaining the benefits of a merger driven by strategy instead of finance requires a thorough integration process."
Paul Esselman, senior EVP and managing director of Cejka Executive Search, said the growing focus on consumerism is an overarching theme behind health systems' reasons for adding to their leadership rosters. In short, according to Lagasse, health care providers are looking "not just on quality, but the overall patient experience."
How to add a new executive role
When health systems add to the executive ranks, it's important for leaders to take the right approach to implementation, Solazzo said—otherwise, "you can create friction and complexity you didn't want, and confusion." In other words, stakeholders say, preparation and communication are critical.
When it comes to preparation, Esselman said a "key element" is "making sure the new role fits into the organization's strategic plan." He explained, "How this individual will help the organization achieve that becomes critical because that ties the new role to the organization. A lot of work up front is well suited to these types of roles."
Solazzo pointed to Northwell's adoption of new C-suite roles as an example of a successful process. When implementing the new positions, the health system adopted a team-oriented approach, Solazzo explained, that sidestepped a more traditional, hierarchical perspective. "We don't focus on org charts," Solazzo said. "We focus on our objectives and how we can accomplish things as a team."
And that commitment to a team approach fosters flexibility, Solazzo added. "If your organization isn't flexible, nimble, innovating, prepared for change, it will not do well in the creation of new positions," he said. "You have to be adaptable in this kind of environment or you die."
Communication surrounding a new role is another key element, Solazzo said. He said when communicating the specifics of the new role, leaders need to convey that the new position "isn't someone taking over a piece of someone else's work, but is viewed as another individual to be part of the team."
Kinslow also touched on the importance of communication, saying the CEO and board in establishing a new C-suite position must "set clear expectations about the new role and communicate those widely, first among the senior leadership team and then more broadly in the organization."
New positions become common—and more are expected to emerge
Esselman said he expects additional new C-suite titles will come into being as health care continues to evolve.
"We're seeing changing delivery models," Esselman said. He added, "As we find a more consumer-driven health care environment, the next generation is coming up and their care and delivery are going to be looked at. You need to be responsible to what the patients' needs are, and that's going to evolve. It will necessitate leaders looking ahead, and saying, how do we take care of these patients in the future" (Lagasse, Healthcare Finance News, 7/14).
Advisory Board's take

Kate Vonderhaar, HR Advancement Center
The expansion of the C-suite reflects the increasing complexity and size of the modern health system. That growth comes with a major challenge: There is now more distance between executives and frontline managers and staff, both literally (in the case of geographically-dispersed health systems) and figuratively (there are more layers between the frontline team member and the CEO). This distance makes it more difficult for frontline managers and staff to interact with executives. And it means every interaction staff do have with executives matters more, since the interactions are likely to be relatively fewer and far between.
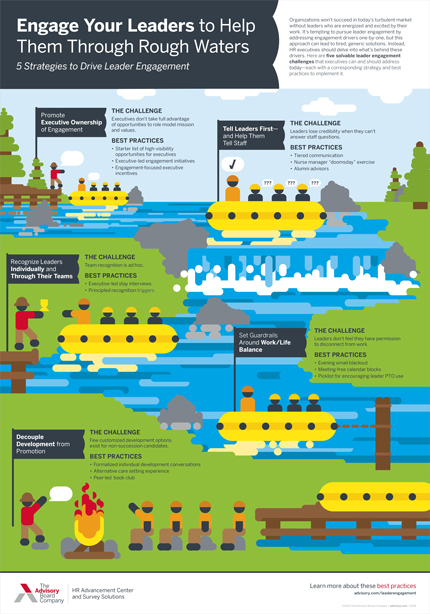
Every executive, regardless of their specific area of oversight, needs to make a concerted effort to be visible and help staff understand the connection between the organization's mission and the work they oversee. Executive rounding is a great place to start—but there's a big difference between rounding and rounding well. To be effective, we recommend executive rounders ask a standard set of questions (such as the sample questions here) and ensure there is a plan in place to quickly follow up on any issues raised by staff. For other ways executives can engage frontline leaders and staff, download our infographic.
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.