Auto logout in seconds.
Continue LogoutAs part of the Affordable Care Act's (ACA) broader effort to ensure health insurance coverage for all U.S. residents, the federal government will pay to expand Medicaid eligibility in every U.S. state beginning in 2013.
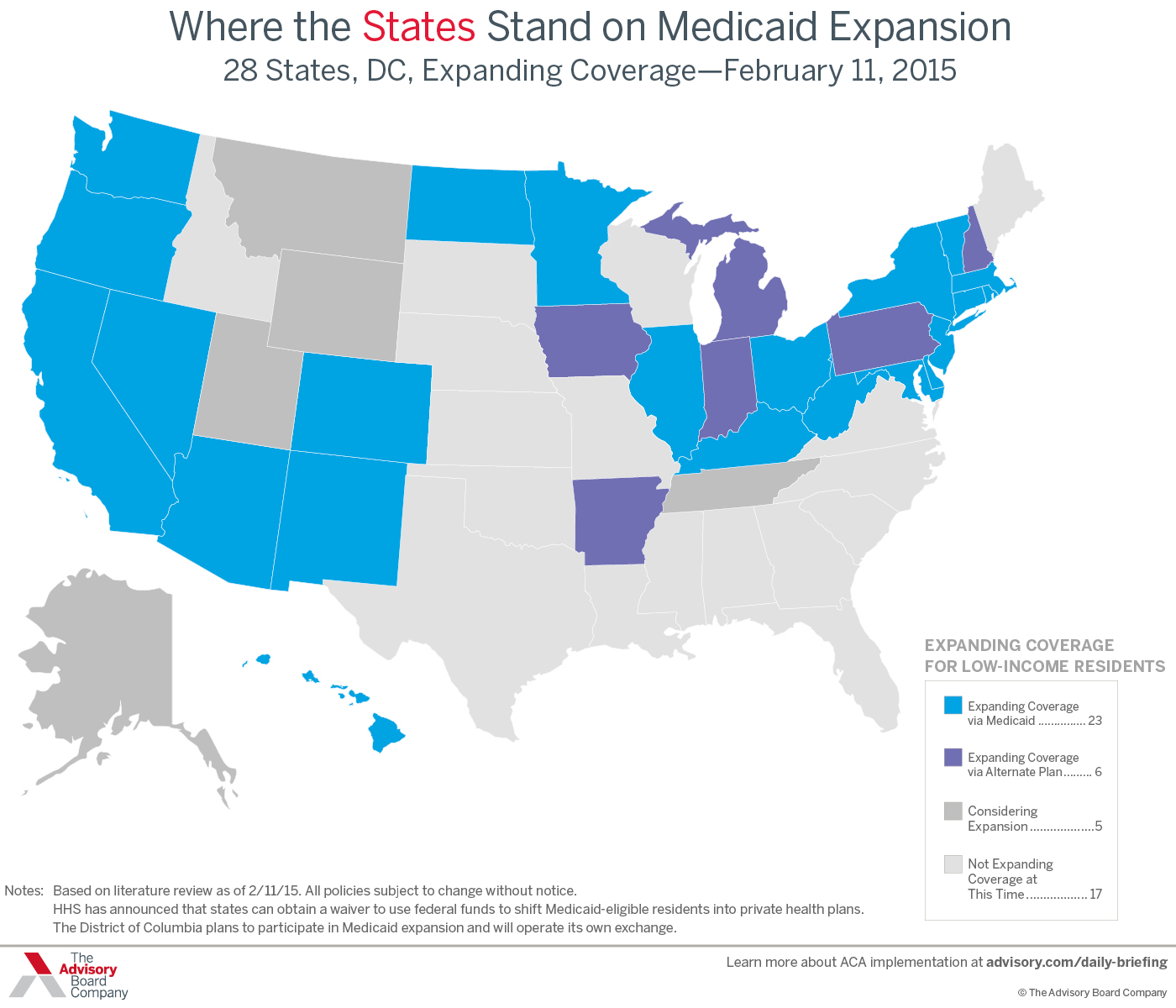
Who is expanding—and who is paying?
From 2014 to 2017, the federal government will pay for 100% of the difference between a state's current Medicaid eligibility level and the ACA minimum. Federal contributions to the expansion will drop to 95% in 2017 and remain at 90% after 2020, according to the ACA.
Which states would save money under ACA's Medicaid expansion?
As the ACA was originally written, states would lose all federal Medicaid funding if they refused to expand their program to the ACA minimum.
However, the Supreme Court in June 2012 ruled that the federal government could not withhold all federal Medicaid funding for states that chose not to expand their programs. The decision effectively allowed state officials to opt out of the expansion, and some have said they will do just that.
Who is eligible for Medicaid under the ACA expansion?
States that participate in the ACA expansion must provide Medicaid coverage to all state residents below a certain income level.
Specifically, participating states must cover all residents ages 19 to 65 who have a household income below 133% of the federal poverty level (FPL), with a 5% income disregard. Effectively, this means that adult residents with a household income below 138% of the FPL would be eligible for Medicaid under the expansion. That's nearly $32,000 for a family of four, and $15,400 for an individual.
Why not just set the official eligibility level at 138% of the FPL? When the Senate passed the ACA in 2009, it set the eligibility level at 133%. However, the House wanted to set eligibility at 150%. Lawmakers said the Senate rules might prevent them from changing the eligibility level during reconciliation, so they decided to keep the Senate-approved 133% eligibility level and include a 5% income disregard.
What is the Arkansas model?
In February 2013, Arkansas Gov. Mike Beebe (D) announced that the federal government would pay for Arkansas to expand health coverage to low-income residents through the state's insurance exchange, rather than its Medicaid program.
Like the ACA Medicaid expansion, the plan will extend insurance coverage to all residents below 138% of the federal poverty limit. (The federal government has said it will not fund any partial expansion models.) Although newly insured residents may face some co-payments, the federal government has agreed to cover the entirety of their premiums for the first three years. As with the Medicaid expansion, the state will then begin increasingly covering a share of the costs, until it reaches 10% of the costs in 2020.
HHS later announced that other states seeking to use federal funds to shift Medicaid-eligible residents into private health plans would have to obtain a waiver from the federal department do to so.
Sources: Medicaid.gov fact sheet, accessed 1/18; Galewitz, Kaiser Health News, 12/5/2012; Washington State Health Care Authority fact sheet, accessed 1/18
Don't miss out on the latest Advisory Board insights
Create your free account to access 1 resource, including the latest research and webinars.
Want access without creating an account?
You have 1 free members-only resource remaining this month.
1 free members-only resources remaining
1 free members-only resources remaining
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
You've reached your limit of free insights
Become a member to access all of Advisory Board's resources, events, and experts
Never miss out on the latest innovative health care content tailored to you.
Benefits include:
This content is available through your Curated Research partnership with Advisory Board. Click on ‘view this resource’ to read the full piece
Email ask@advisory.com to learn more
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.
Benefits Include:
This is for members only. Learn more.
Click on ‘Become a Member’ to learn about the benefits of a Full-Access partnership with Advisory Board
Never miss out on the latest innovative health care content tailored to you.